If you’re reading this article, then we’ve probably piqued your interest. So, what do dental implants and gum disease have in common? Here’s what you need to know in a nutshell.
- Gum disease can lead to tooth loss
- Tooth loss is treated with dental implants
- Healthy gums are essential to receive implants
- A patient can develop gum disease even with a dental implant
- Gum disease can cause a dental implant to fail
Let’s take a closer look at gum disease and dental implants.
What is gum disease?
Gum disease, also known as periodontal disease, is a severe but, sadly, common gum infection caused by bacteria-laden plaque forming on the teeth around the gumline. In its early stage, it’s referred to as gingivitis and can be treated with a professional dental clean and improved oral care at home. Yet, a recent report shows that only 50% of the adult population brush their teeth twice daily.
Without treatment, it can escalate to a more severe gum infection – periodontitis – that damages the soft tissues and destroys the bone holding the teeth in place. Periodontitis can cause gum recession, leading to loose teeth that eventually fall out.
However, a person can have periodontal disease without presenting any symptoms. In fact, it’s reported that 1 in 4 adults has a periodontal disease with periodontal pockets exceeding 4mm. This highlights the need to attend regular dental check-ups with your dentist to keep your oral health in check.
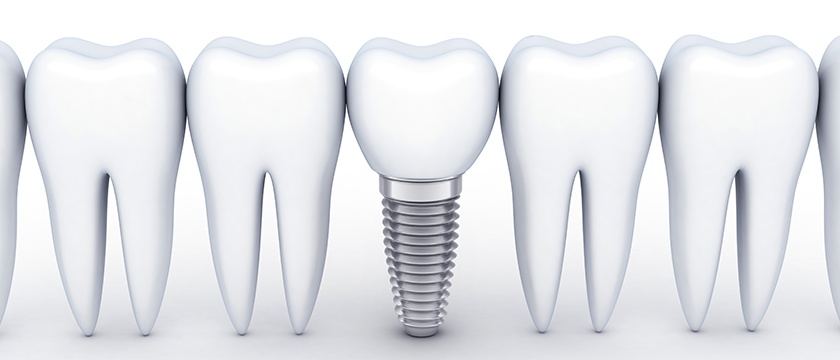
What are dental implants?
Dental implants are the gold standard of tooth replacement. Dentists recommend them as a tooth replacement solution for patients who have had teeth extracted due to gum disease, infection, or trauma; Or for those wanting to replace teeth missing for years to eliminate or retain dentures.
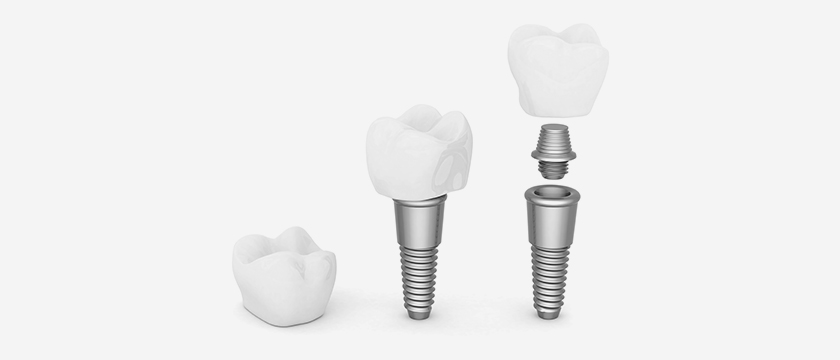
Implants replace the entire tooth structure. During a short surgical procedure, a titanium post is implanted (anchored) into the jawbone. Over time, the implant fuses with the soft tissue and bone to act as an artificial tooth root. The foundation becomes strong enough to then support a false tooth or dental crown. Because the porcelain crown is colour matched to the shade of the natural teeth, it blends seamlessly into the smile.
- Prevention of bone loss
- Ability to bite and chew food more easily
- Stability and durability
- Natural appearance
But just like with natural teeth, decay and gum disease can cause an implant to fail.
Hopefully, you are starting to understand the correlation between dental implants and gum disease by now.
Will I lose my teeth if I have gum disease?
Gum disease is the leading cause of tooth loss, but there’s no need to assume you will lose a tooth when you have a diagnosis. You can discuss your concerns during a consultation with your dentist.
Provided the problem is addressed speedily, there are treatments available and habits a person can adopt to reverse gingivitis and avoid tooth loss.
Tooth loss takes place when soft gum tissue is severely damaged. A lack of healthy gum tissue enables bacteria to penetrate deeper into the mouth, destroying the bone holding teeth in place.
Losing a tooth to periodontal disease is the worst-case scenario but do your best to avoid reaching this stage of infection. If you notice your teeth feel loose, then get in contact with our experienced dentists right away.
Does gum disease go away if a tooth is extracted?
If tooth loss seems inevitable, it’s best to have your dentist extract the tooth. However, removing the tooth doesn’t mean gum disease disappears. Without treatment, periodontal disease will spread, potentially causing further tooth loss.
Moreover, if you lost a tooth due to injury or an accident and didn’t have periodontal disease at the time, the missing tooth can increase the risk of developing the disease. When a tooth is missing, gums and bones begin to weaken, recede, and dissolve, creating periodontal pockets where bacteria can accumulate and thrive.
If you are missing a tooth, it’s essential to discuss tooth replacement options at a consultation with your dentist. However, if you have gum disease, you need to deal with one issue at a time.
How gum disease is treated
Depending on the stage of periodontal disease, dentists provide several treatments, which include:
Non-surgical gum disease treatments for early-stage gum disease
- Scaling
- Antibiotics
- Root planing
Surgical treatment for severe gum disease
- Pocket reduction
- Bone grafting
- Guided tissue regeneration
- Tissue stimulating proteins
Can I have dental implants if I have gum disease?
The straightforward answer to this question is no. Implants must be placed into the healthy dense bone, and as we’ve mentioned earlier, periodontal disease weakens and dissolves gum tissue and bone. So, even after gum disease treatment, your gums and bone may not be strong enough to support a dental implant. This being the case, you may be an ideal patient for a bone graft to generate new bone, enabling you to have dental implants at a later date.
What will happen if I get gum disease after a dental implant?
If you allow your oral hygiene to slip, you could develop another form of gum disease – peri-implantitis.
This condition occurs when bacteria build up around the bone and soft tissue supporting the implant. Symptoms include:
- Swelling
- Bleeding
- Bad breath
- Loosening implant
The worst-case scenario is the implant loosens and falls out. However, treatments are available should you develop peri-implantitis to halt the disease and stabilise the implant.
Do you have any further questions about dental implants and gum disease?
At DDSS/DDI, we pride ourselves on delivering high quality, friendly dental care. We adopt a preventive approach to help you avoid gum disease from the start.
Our dentist has invested in the latest technologies and techniques to diagnose and treat gum disease. We also provide the latest digital dental implants and same-day dental crowns if an implant is necessary.
Why not schedule a free dental implant consultation with the team at DDSS/DDII today.
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner
Reference
Dental Report Finds Only Half Of All Australians Brush Their Teeth Twice A Day
Australia’s Oral Health Is Getting Worse … And Covid Is Not Helping
https://www.ada.org.au/News-Media/News-and-Release/Media-Releases/DHW-2020-media-release-31072020
Oral Health – Gum Disease
https://www.cdc.gov/oralhealth/fast-facts/gum-disease/index.html
What to Know About Periodontal Pockets
https://www.healthline.com/health/periodontal-pockets
Science Direct – Peri-implantitis explained
https://www.sciencedirect.com/topics/medicine-and-dentistry/peri-implantitis
Peri Implantitis – Treatment Options
https://www.oralhealthgroup.com/features/peri-implantitis-treatment-options/